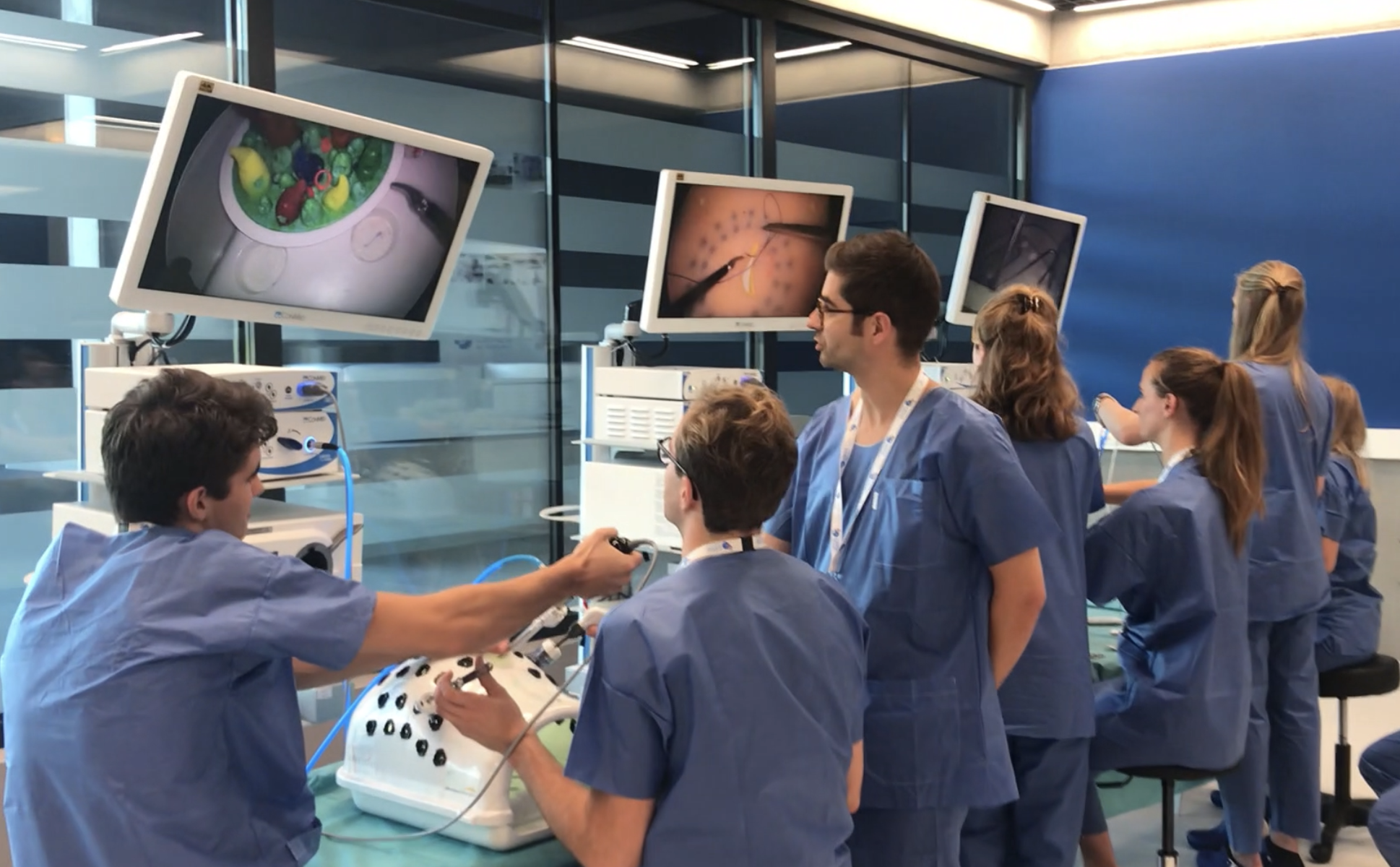
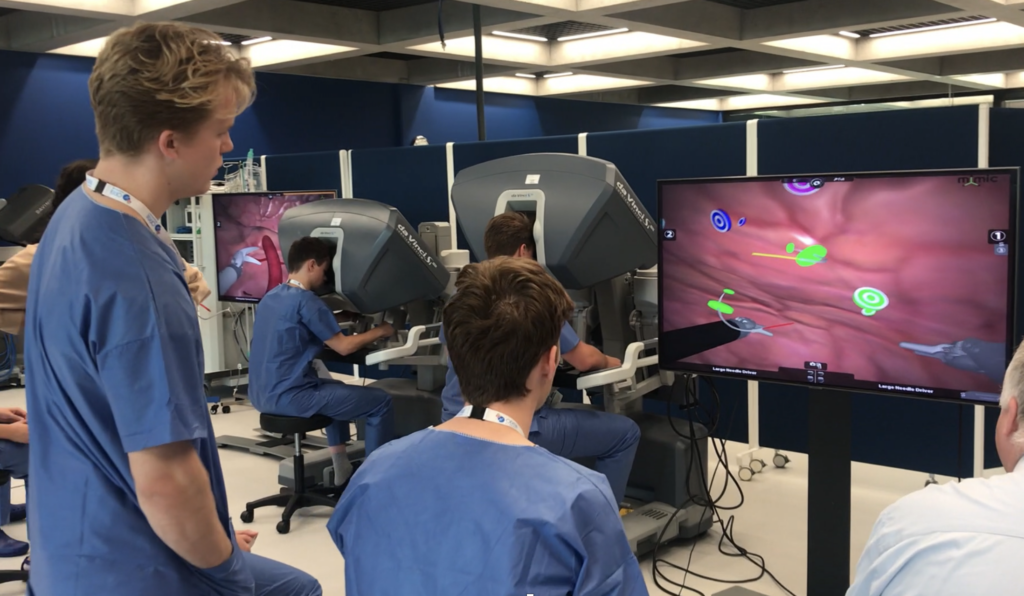
Medical education with Virtual Reality (VR)
Virtual Reality (VR) is a technology that can provide authentic and immersive learning environments using VR headsets. By simulating different medical scenarios, it provides possibilities to educate students on a large variety of topics and practical skills, in a safe and accessible learning environment.
Multiple applications and (interactive) 360-degree videos were developed by a multidisciplinary team:
- “Virtual Ward” (App)
This app consists of an interactive virtual tour of a hospital ward, in which learners explore the Internal Medicine ward and learn about the roles of different health care professionals and their mutual interactions. In each room, the learners listen to a voice-over and look at hotspots to gather additional information.
Further information can be found in this publication. - “Urosepsis” (App)
This app consists of an interactive video of an emergency situation at the urology department. Students are able to observe this situation in a safe environment and answer related questions.
More information about this app can be found at the website of Leiden Learning & Innovation Center. - “(Un)professional Behavior” (360° video)
Short video of a fictive hospital ward round in which the Code of Conduct for Doctors [1] is violated. This is used to make students aware of the Code of Conduct and to promote action against practices of unprofessional behavior in the clinic.
For further information seethis publication. - Kidney Donation and Transplantation (360° video)
A 360° video of a kidney transplantation procedure. Students of different levels use this video to study collaboration skills, communication skills or the procedure itself.
Further information on the development of this video can be found in this publication.
Further reading on the development of these apps can be found in this publication.
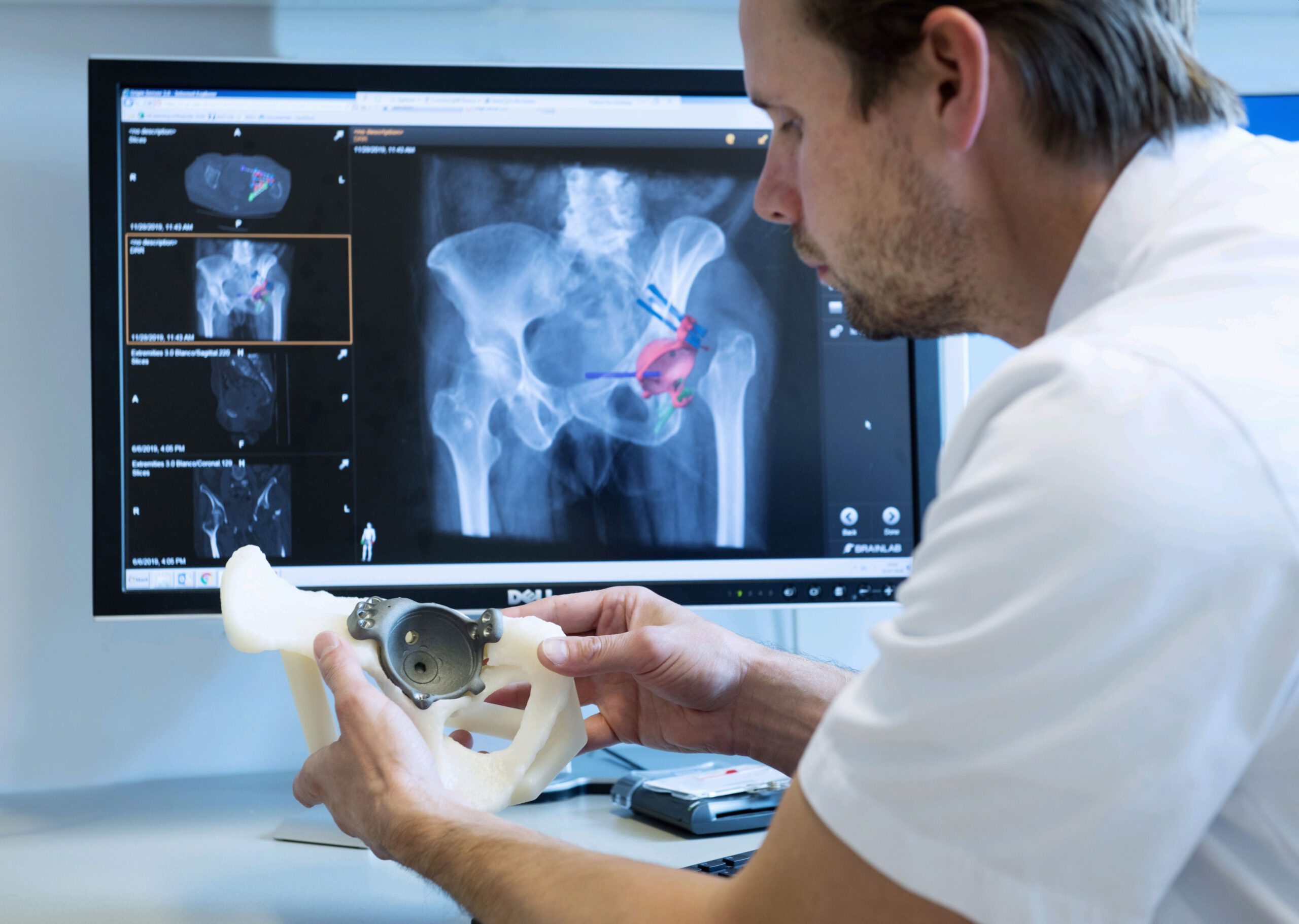
Medical education with Augmented Reality (AR) / Mixed Reality (MR)
Augmented Reality (AR) and Mixed Reality (MR) are immersive technologies that enhance our perception of the real world by overlaying digital content onto it. This augmentation is typically achieved through the use of devices like specialized headsets or smartphones equipped with cameras and sensors. While AR is for observational purposes only, MR allows the user to also interact with the virtual environment.
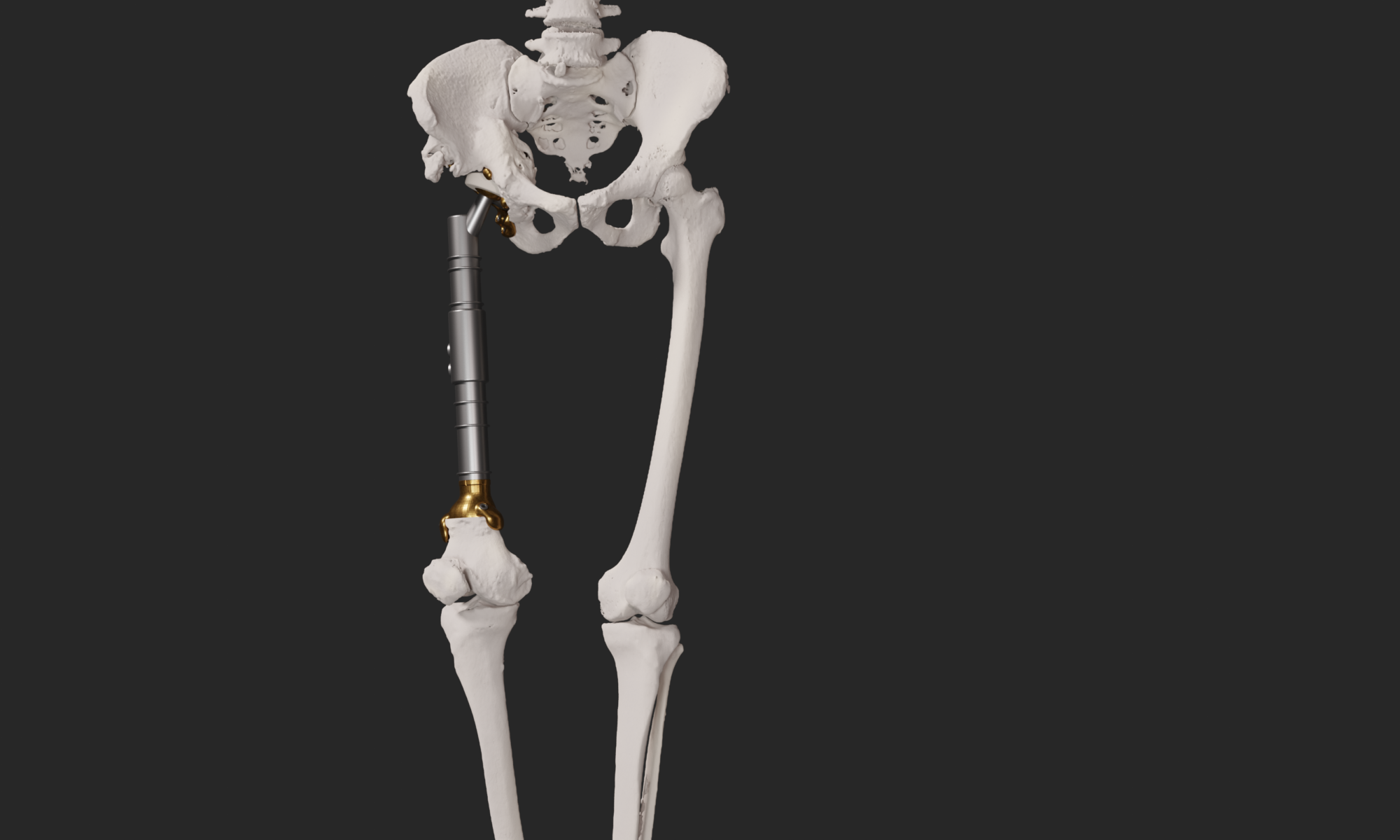
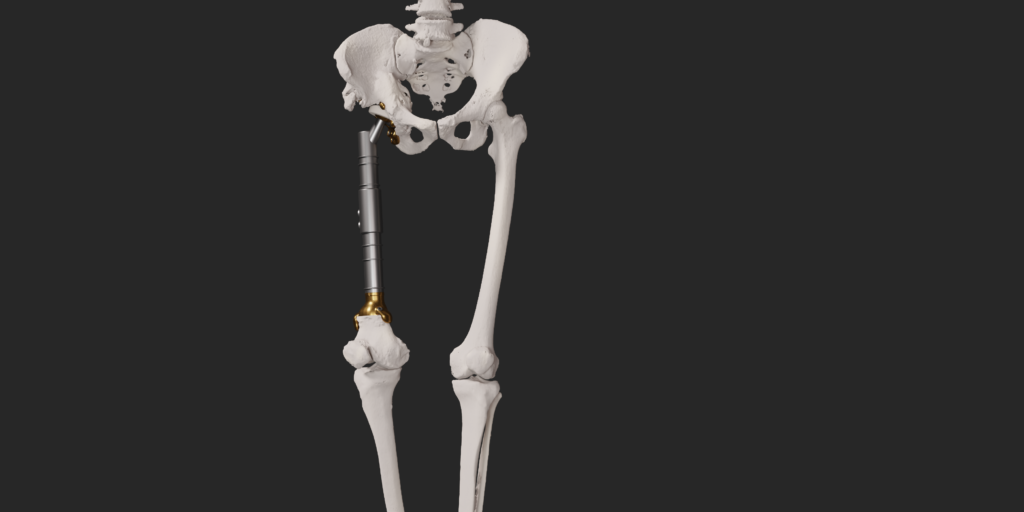
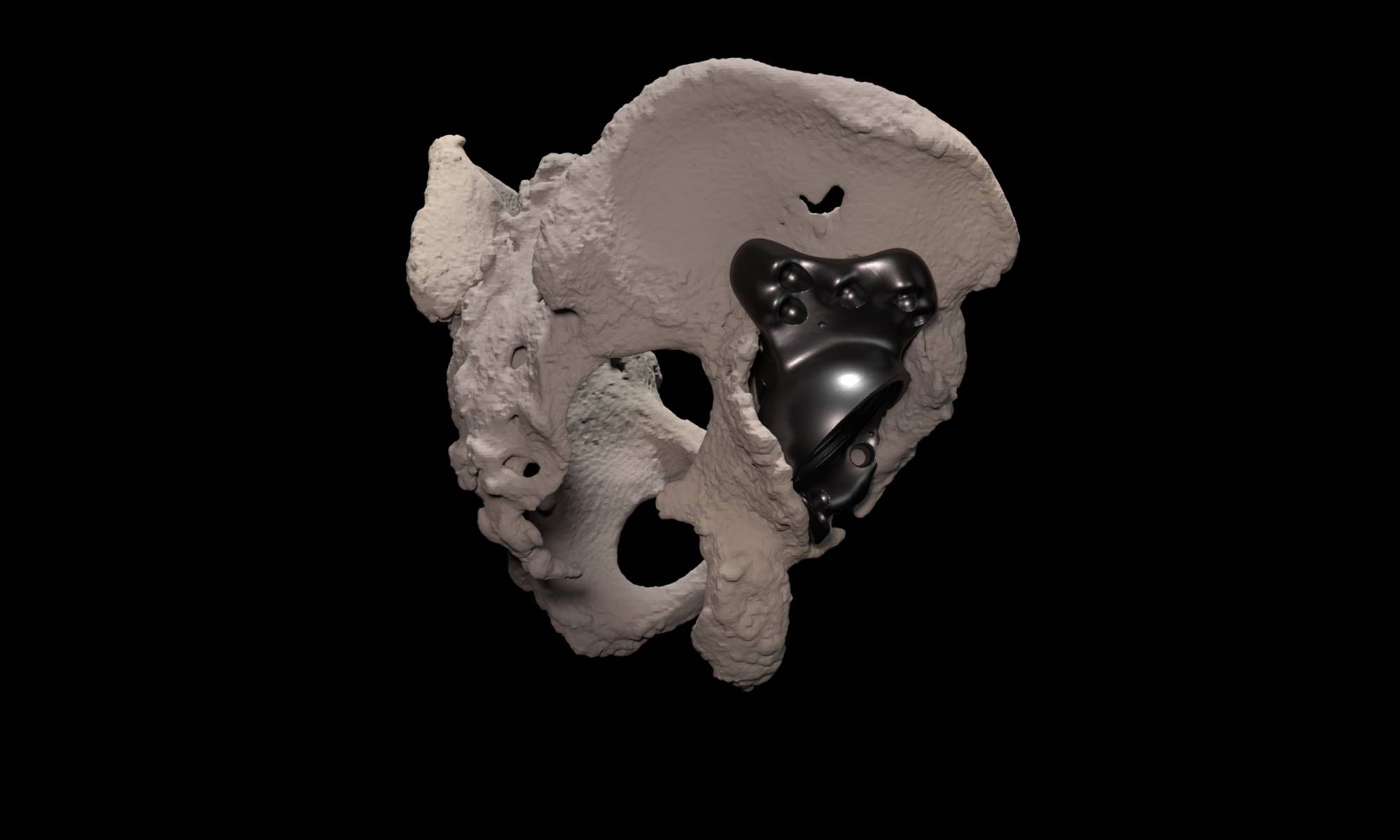
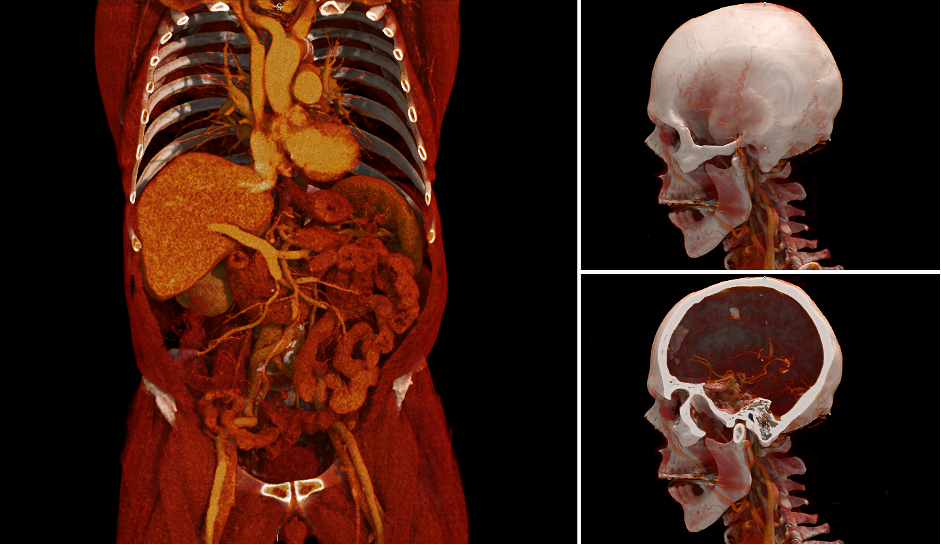
Within medical education, AR and MR can be effective learning tools, offering immersive and interactive experiences for both students and healthcare professionals. One notable application is the use in anatomy related education. Traditional learning methods often involve static images and textbooks, which may not provide a comprehensive understanding of three-dimensional structures. AR and MR, however, allow students to visualize and interact with detailed 3D models of the human body, facilitating a more dynamic and engaging learning experience.
In recent years, various apps were developed that are currently used in our medical education:
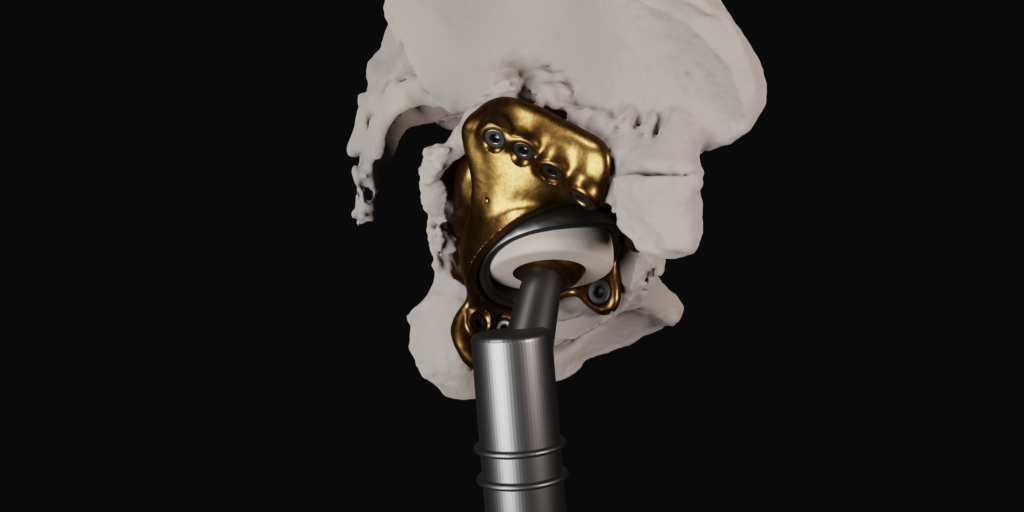
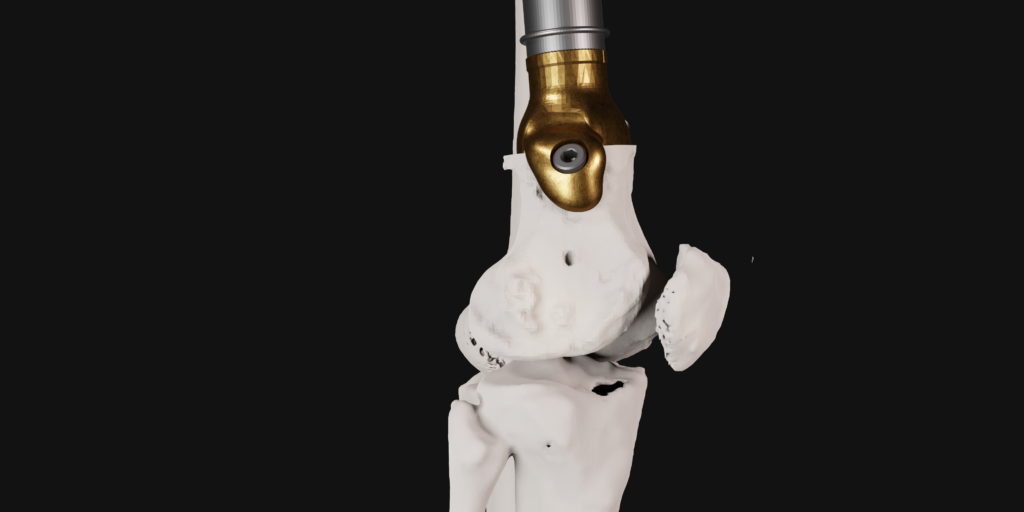
- AugMedicine: Transplant cases
This app focuses on enhancing learners’ understanding of the spatial relations between 2D CT scans and 3D anatomical models. To achieve this, the app visualizes CT scans on a virtual plane that intersects the 3D model at the same location as where the CT image was taken.
More information about this app can be found at the website of Leiden Learning & Innovation Centre. - AugMedicine: Lung Cases
An MR app on the clinical presentation of shortness of breath (dyspnea). This application shows a 3D model of the human thorax on which different cases of dyspnea can be displayed. Users can manipulate a virtual stethoscope to listen to the lung sounds at different locations and from different angles.
More information about this app can be found at the website of Leiden Learning & Innovation Centre.
More information about the development and user experiences can be found in this publication. - AugMedicine: Ultrasound
Our newest application focuses on cardiac ultrasound, featuring a detailed 3D model of the heart. It enhances anatomy and physiology learning, offering a virtual environment for practicing ultrasound skills, and improving hand-eye coordination.
More information can be found inthis publication.
These applications were co-created with Leiden Learning & Innovation Centre.