Current techniques for producing tablets are mostly incapable of filling the gap between ‘one size fits all’ and individualized pharmaceutical treatment options. 3D printing allows the small-scale production of tailored dosage forms, precision dosing, polypills and optimized drug delivery. At the Department of Clinical Pharmacy and Toxicology, 3D-printed tablets are produced. With our research, patients can hopefully benefit from this novel personalized treatment as soon as possible.
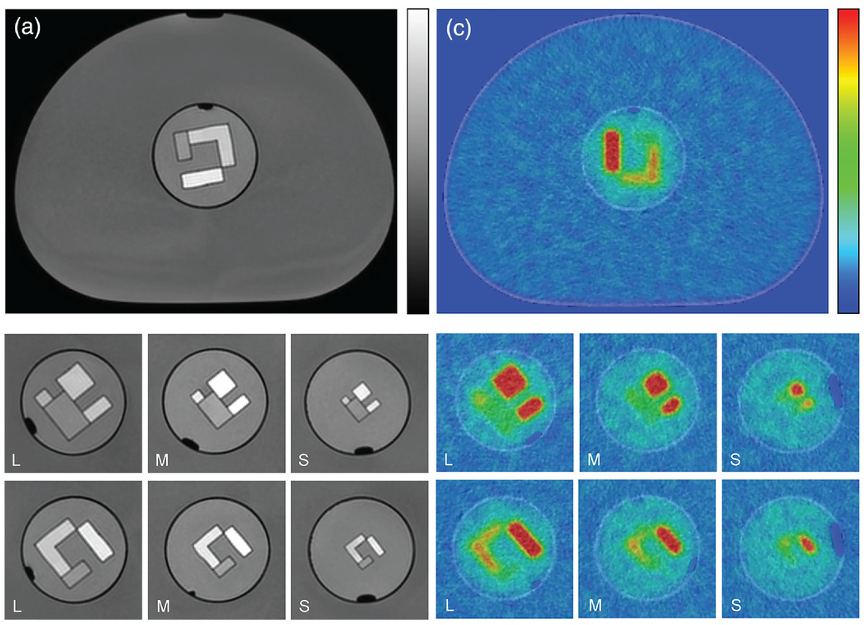
Multimodality imaging phantom
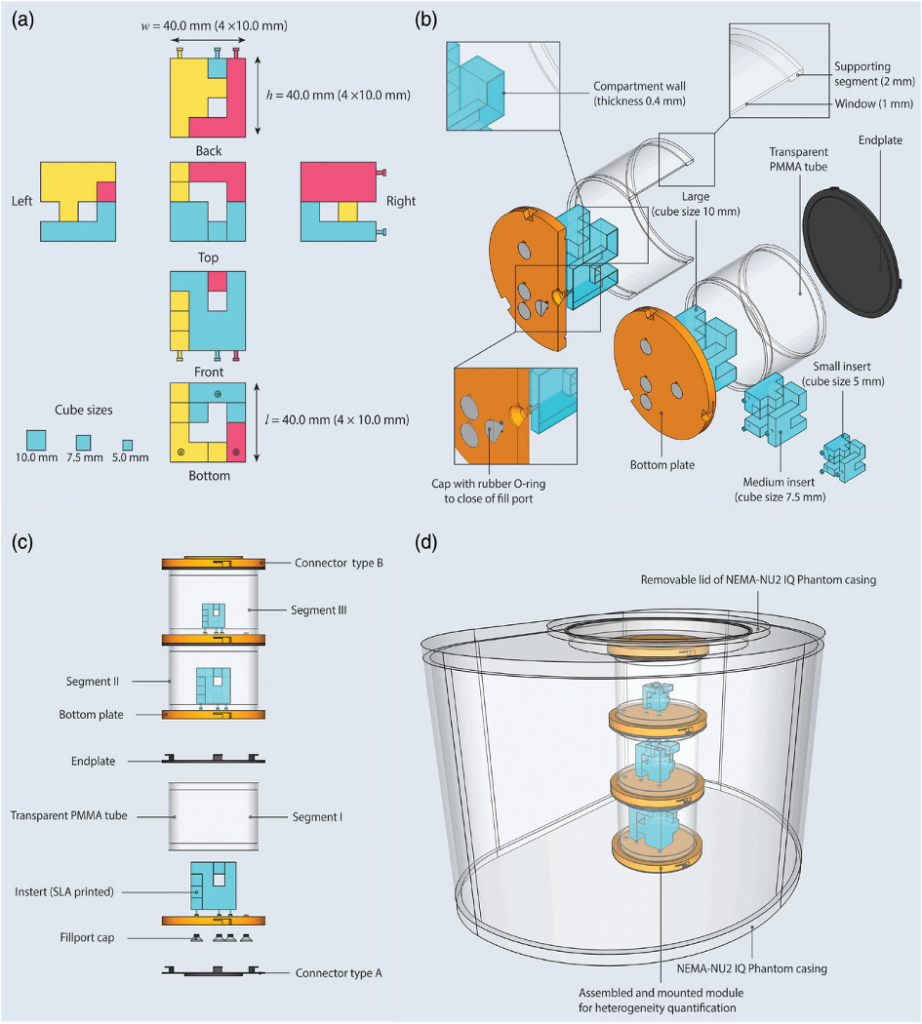
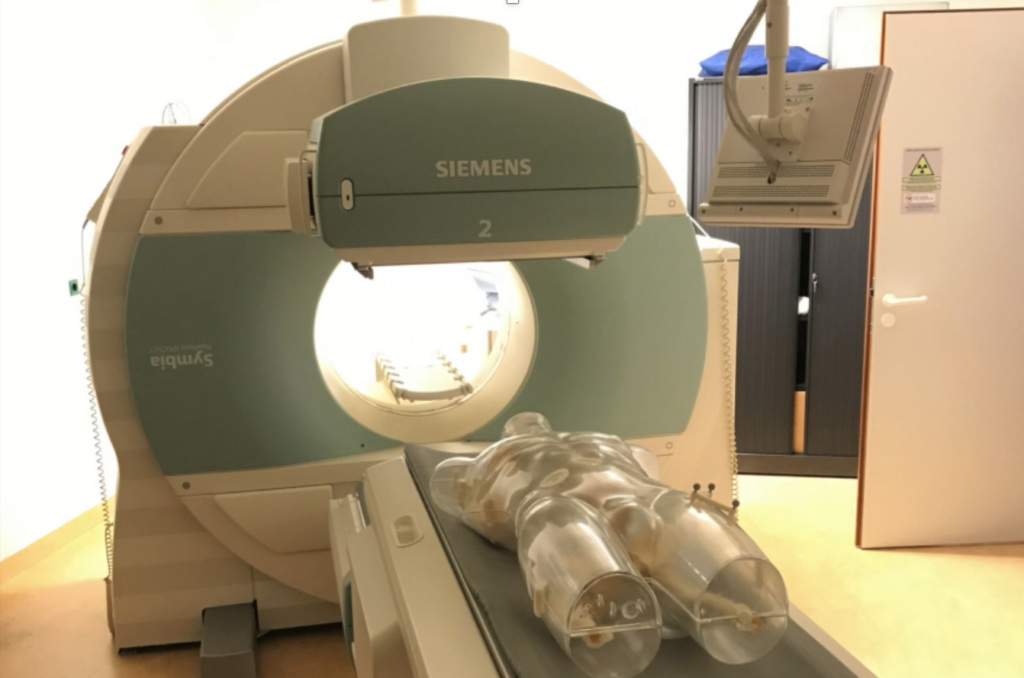
Medical imaging has a pivotal role in clinical management of oncology patients. Over the past years, the ability to characterize cancer lesions has improved with the advent of hybrid imaging techniques, where X-ray computed tomography (CT) and magnetic resonance (MR) imaging are combined with PET and or SPECT. An important aspect of this characterization is the accuracy, precision and repeatability of imaging features under different imaging conditions. Simulation of different imaging conditions is typically achieved by performing standardized experiments using phantoms. We designed and developed a multimodality imaging phantom to allow testing of features in hybrid imaging. Our research showed that the fantom permits the simulation of heterogeneous uptake and enhancement patterns in the most commonly used tomographic imaging modalities in hybrid imaging and provided insight differences in image quantification between modalities.
Phantoms for robotic surgery
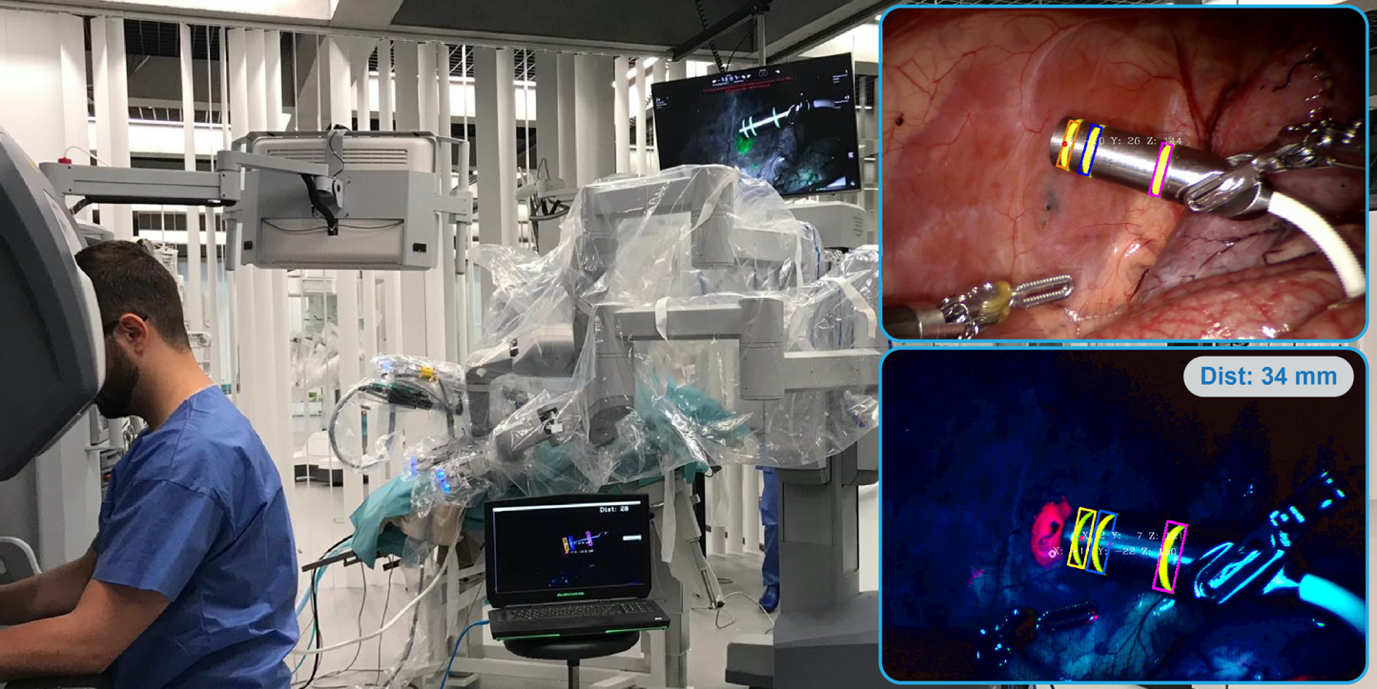
To investigate new image-guided surgery technology for a minimal invasive robotic setting, phantoms are created that are compatible with various forms of medical imaging and allow for the surgical robotic platform to be docked, simulating the eventual surgical application.
Click-On fluorescence detectors
The aim of this study was to engineer ‘click-on’ fluorescence detectors that transform standard robotic instruments into molecular sensing devices that enable the surgeon to detect near-infrared fluorescence signals in tissue grasped during every part of the surgical procedure. When used in combination with fluorescent tracers, this allows for a first step towards tissue characterisation via the surgical instruments themselves.
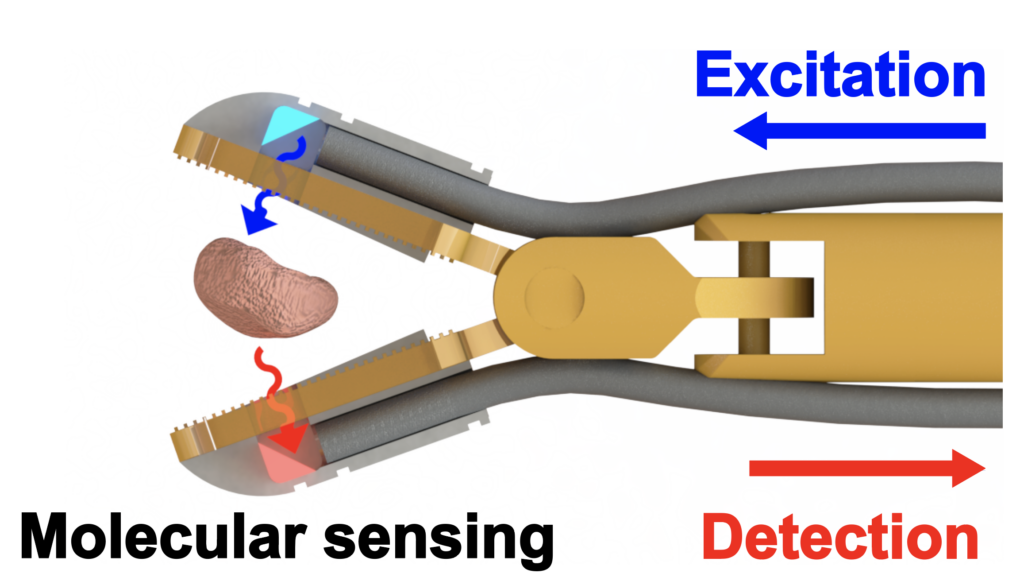
Surgical Instrument Tracking
Decision-making and dexterity, features that become increasingly relevant in (robot-assisted) minimally invasive surgery, are considered key components in improving the surgical accuracy. In this project, motion tracking is used to study the added benefit of a novel tethered gamma detector.
Optical navigation of DROP-IN probes
With translation of the DROP-IN gamma probe, radioguidance has advanced into laparoscopic robot-assisted surgery. Since it is not always trivial to locate preoperatively marked lesions during surgery, especially when using tumor-targeted tracers such as 99mTc-PSMA I&S, surgical navigation can further enhance the translation between planning at the dept. of nuclear medicine and the actual treatment in the operating room. In this project, a method is generated to navigate a DROP-IN probe during surgery using optical (fluorescence) techniques.
Freehand Fluorescence tomography for image-guided surgery
Within image-guided surgery, ‘hybrid’ guidance technologies have been used to integrate the complementary features of radioactive guidance and fluorescence guidance. In this project, a novel freehand fluorescence imaging and navigation approach was generated to complement existing freehand SPECT modalities in a hybrid setup. Combined the freehand technologies render a unique hybrid imaging and navigation modality that exploits the strengths of the individual technologies.
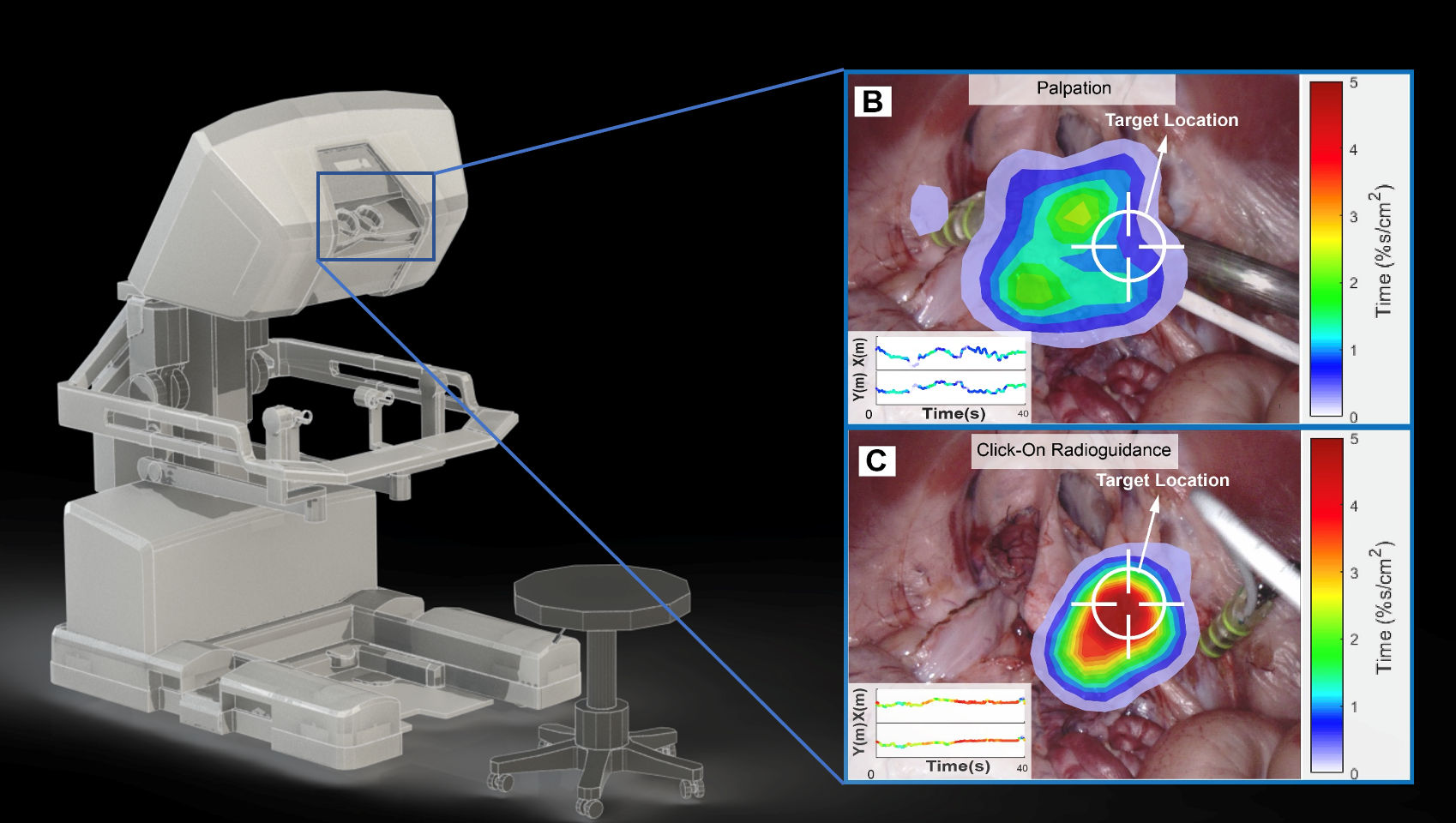
DROP-IN gamma probe
In oncology, radical surgical resection of cancerous tissue is one of the most efficient forms of treatment. For accurate lesion localization during surgery, image-guided surgery methods play an ever-increasing role. Such methods predominantly rely on radio- and/or fluorescent-tracers to ‘illuminate’ targeted tissues, e.g., sentinel lymph nodes (ICG-99mTc-nanocolloid) and PSMA-positive tumor (99mTc-PSMA I&S). To optimally integrate radioguidance during robot-assisted surgery, a tethered and miniaturized gamma detector for wristed robotic instruments, the so-called DROP-IN gamma-ray-detection probe was engineered. This has resulted in two commercial products that are now CE-marked for routine clinical use (Crystal Photonics GmbH and LightPoint Medical). In one of our most recent clinical studies on this topic, the DROP-IN proved to be superior to the use of fluorescence guidance and rigid laparoscopic gamma probes.